|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
The Effect Of Social Isolation And Loneliness On The Health Of Older Women |
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
M. Hall & B. Havens Introduction Social isolation and loneliness are often considered to be problems of growing older. As people age, many outlive relatives and friends, and social interaction may become limited as people stay closer to home because of mobility difficulties and increased chronic illness. Older individuals may be more or less dissatisfied with the narrowing of their social network; and for those who are dissatisfied, the result is feeling lonely. Researchers and practitioners tend to agree that social isolation and social loneliness among older people are often related to living alone and being in poor health. The question that remains is the relationship among isolation, loneliness, health and well being. An important related issue is what steps might be taken with older persons to alleviate isolation and loneliness. To address these concerns, a partnership was formed between academic researchers at the University of Manitoba and five community organizations. Survey and health services utilization data were analyzed using constructs of social isolation and social loneliness as outcome measures. Preliminary information from these data analyses were presented at a series of six public forums to raise awareness of potential concerns and to encourage discussion at the community level of ways to address these concerns. Review of the Literature Social isolation is an objective measure of social interaction, while social loneliness is considered to be the subjective expression of dissatisfaction with a low number of social contacts. Social isolation is sometimes referred to as aloneness or solitude. Those who are often alone, however, are not necessarily lonely, as solitude can be a personal choice. Social loneliness is defined as negative feelings about being alone, and as such is an experience that occurs irrespective of choice. Social loneliness, then, can be thought of as negatively perceived social isolation. As a social concept, then, loneliness emphasizes the importance of social perceptions and evaluations of an individual’s personal relationships. It includes those situations where the number of existing relationships is smaller than an individual finds desirable or acceptable. It is possible, then, for two persons with the same number of social contacts to perceive these contacts differently. Therefore, one person may express social loneliness while the other does not. Studies have found rates of loneliness in older populations to range from 20% - 60%, and many researchers have noted associations with poor health and well being. Some, for instance, have found that older individuals who are very lonely are at increased risk for nursing home placement. Others have found that a poor self-rating of health distinguishes those who are lonely in older age from those who are not, and psychological well-being has generally been seen to be related to a supportive social network. What is not clear, however, is whether loneliness results from decreased contacts with other people due to ill health, or if decreased contact and the possibility of loneliness precede ill health. What appears fairly certain, however, is that the isolation and loneliness that may accompany aging are relevant issues for older women. Women are more vulnerable to higher levels of loneliness, in part, because of their greater longevity compared to men. As women age they often outlive spouses, friends and family members who previously provided the social and emotional support that are important for health and well-being. Women are also more likely to be widowed, live alone, and to experience an increased number of years with declining health. Many older women live with multiple chronic health conditions that can limit mobility and thus further restrict their capacity to socialize. Older women also live with increased risk of institutionalization and, it has been suggested, higher rates of emotional distress when compared to older men. Objectives For this study, researchers at the University of Manitoba partnered with five community organizations dedicated to the well-being of older Manitobans: Age and Opportunity Centre Inc., Creative Retirement Manitoba, Manitoba Society of Seniors, Seniors’ Community Resource Councils, and the Victorian Order of Nurses of Winnipeg. Wehad three major objectives:
The first two objectives were met by analyzing data from the Aging in Manitoba Study (AIM), which contains measures of social isolation and social loneliness as well as sociodemographics, health status, and health utilization for a representative sample of older adults. The last objective was met by presenting preliminary data in a series of public meetings to encourage discussion and elicit recommendations for ways to address isolation and loneliness among older people. Our study was conducted within the framework of population health. This perspective views social isolation and social loneliness as determinants of health status. That is, these factors have the potential to influence health and well-being, access to health care, and the effectiveness and outcome of the care received. This view encompasses a broad definition of health, including social, emotional, cultural, spiritual and physical influences, and acknowledges the sociopolitical and economic context of the lives of older individuals. As an example, a widow who has outlived most of her peers and lives at a distance from her remaining family usually eats alone, and grocery shopping may be a major undertaking. Therefore, she may cook infrequently and eat less nutritious meals, making her a ready host for infections and flu. Her situation may also tend to erode her self-esteem and self-confidence, making it more difficult for her to seek appropriate health care or to follow through with recommended treatment. The Sample The sample for our study was derived from the 1996 panel wave of the Aging in Manitoba (AIM) Study. The participants were originally interviewed for cross-sectional studies that occurred in 1971, 1976 and 1983. Follow-up surveys were conducted in 1983 (for survivors of 1971 and 1976), in 1990, and in 1996. All individuals who could be re-contacted were interviewed in person. Information for those who could not participate in an interview because of illness, inability to hear the questions, or cognitive decline was obtained from proxy individuals if possible. All waves of the AIM study have included sociodemographic and health status information. The data also include health utilization for provincially insured services: physician visits, hospitalizations, residence in personal care homes, use of home care services, and purchase of prescription medications. Responses to the questions measuring social isolation include factual information only, such as the number of individuals a person interacts with on a regular basis. These questions could be answered by participants or by proxy individuals. Only participants, however, could provide answers to questions measuring thoughts and feelings, such as those included in the measures of social loneliness. Therefore, the total number of cases available for analysis differed depending on the type of measure used. The 1996 wave used for this study included 1,868 individuals whose minimum age was 72. Forty percent of the sample was male and 60% was female, typical of the gender distribution of this age group in Manitoba at the time of interview. Those residing in nursing homes comprised 13.6% of the sample. Forty-five percent of respondents lived in urban areas (Winnipeg and Brandon), and 55% in smaller rural or northern communities or in remote areas. Participatory Research Process Our study involved the combined efforts of researchers, community partner groups dedicated to the health and well-being of older people, and the public. This type of participatory process was designed to provide study results to those most affected by the issues. The roles of the partner organizations were to help define the research
questions, discuss preliminary findings from the data, arrange and assist
with the public presentations, and review the final study results with
regard to the importance and application of the findings. The researchers
conducted the data analyses, documented the findings, and presented
the information to the public. Results of Objective 1: Exploration of gender differences Fifteen items that measure social isolation were explored through bivariate analysis of the AIM data (Table 1). It was found that the women ranked higher than the men on twelve of the items. In particular, the women in the sample were three times more likely than the men to be widowed, and were twice as likely to live alone. Women also ranked higher in terms of perceived financial difficulties, living far away from relatives, having made recent moves to different housing, having a greater number of chronic illnesses, longer stays in hospital, and declines in cognitive status. The women were also more likely to receive a rating of extremely isolated on the Life Space Index, a multiple-item scale that measures overt social interaction. Included within this index are the numbers of regular contacts with family, friends, neighbors, co-workers, and other people seen regularly for specific purposes. The men in the sample ranked slightly higher than the women in residence changes of more than one day from their previous home (a difference of only 0.8%), feeling that older people are seldom active in their community (a difference of 1.3%), and expressing a low level of life satisfaction (0.3% greater the women).
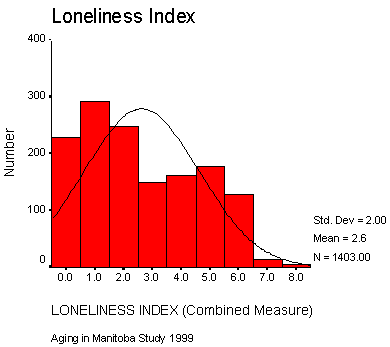
The Loneliness Index used in our study is a composite of the Loneliness Scale developed by researchers in the Netherlands, and two single item loneliness questions from the Netherlands NESTOR studies on aging. The Loneliness Scale is comprised of 11 items, 5 of which measure feelings of belonging or sociability, and 6 items measuring aspects of missing relationships. These items have been found to accurately measure social loneliness in older populations. Chart 1 below shows the distribution of our study sample on the combined measure of the Loneliness Index. Using the Loneliness Index, we found that the proportions of men and women in the sample who expressed any degree of loneliness was similar; i.e., 82% for men and 85% for women. However, there was a greater proportion of men in the not lonely and somewhat lonely groups, and a greater proportion of women in the quite lonely group. In other words, 50% of the women, compared to 39% of the men, could be considered quite lonely. In reference to our first objective then, we found the women in the sample were more socially isolated than were the men, and a greater proportion of the women expressed the highest level of loneliness. We also found that those who were widowed were more likely to express higher levels of loneliness than those who were married, with the women being especially disadvantaged in the area of marital status because more of them were widowed. Similarly, we found that those who lived alone were more likely to be lonely. Again, the women were more disadvantaged because more of the older women in our sample lived alone than did the older men. Consequently, we concluded that gender differences were evident in the experiences of both social isolation and social loneliness in our sample. Chart 1
Results of Objective 2: Relationship of social isolation and loneliness to the health of older women For our second objective, we conducted bivariate analyses of loneliness with various components of social isolation using only the females in our sample. We found that social loneliness was more evident for those women who:
From the health utilization data, we also found that higher levels of loneliness were more likely for women who had:
The results were confirmed by correlational analyses of these variables with the Loneliness Index and the Life Space Index score as a proxy measure for social isolation. All correlations were significant (p less than or equal to .05), except for hospital admissions with the Loneliness Index, and hospital admission, days in hospital, and physician visits with the Life Space Score. We also explored the influence of the Life Space Score on the level of loneliness using backward stepwise logistic regression. The results were significant (p less than or equal to .001), with an unadjusted Odds Ratio (few contacts) of 1.4. In other words, exclusive of other influences, those who have few social contacts (as measured by the Life Space score) are almost half again (1.4:1) as likely to be lonely as those with many contacts. Additionally, we explored the association of gender with the Loneliness Index and the Life Space score. Both associations were significant (p less than or equal to .001). The (unadjusted) Odds Ratio for loneliness is 1.28 (women), and 1.45 (women) for Life Space. We were thus able to conclude that the women in our sample, when compared to the men, were almost one-third more likely to be lonely, and half again as likely to have few rather than many social contacts. Two sets of logistic regression were performed to explore the influences of sociodemographic characteristics and health status on the Loneliness Index and Life Space. The results of the analysis using loneliness as the outcome measure produced six significant independent factors when adjusting for all others. The odds of being lonely were more than double for those who lived alone versus those who lived with others, and about 1.4 times greater for those who felt their health was poor, who were widowed, or who had few social contacts. Having more than four chronic illnesses was also a significant influence, as was evidence of limited functioning. Because these factors are independent, they are additive. The result, then, is that a widow who lives alone, sees few other people and feels her health is poor would be almost six-and-a-half times more likely to be lonely than a married individual who lives with a spouse, sees many people on a regular basis, and is in good health. While female gender was not found to be a significant influence on loneliness, the implication from the bivariate analyses is that the women in the sample were more likely than the men to be lonely because more of the women lived alone and were widowed. Also, as stated previously, the comparison of social isolation by gender shows that women experience greater levels of social isolation than do men on most components. The results of the second regression analysis with the Life Space Index score produced four significant independent factors. The odds of being socially isolated (having fewer contacts) were 1.7 times greater for women than men, 1.3 times greater among those who were older with poor self-rated health, and 1.1 times greater for those with more chronic illness. An accumulation of these effects would mean that a woman over age 80 and in poor health would be almost five-and-a-half times more likely to be socially isolated than men younger than age 80 and in better health. Also, when controlled for age and chronic illness, women over age 80 who rated their health as poor were nearly three times as likely to be socially isolated as women aged 72 – 80 who rated their health as good. The AIM dataset includes health utilization for the year following
the interview as well as the year prior to the interview. These measures
allowed us to test whether loneliness and social isolation in 1996 could
predict use of services one year later. Bivariate correlations with
the health care use variables showed that only the use of home care
services was significant. A logistic regression model using home care
use as the dependent variable showed that both loneliness (Odds Ratio
= 1.66) and few social contacts (Odds Ratio = 1.73) were significant
predictors of home care use when adjusted for age and gender. In other
words, those in our sample who were lonely or had few contacts were
more than one-and-a-half times as likely to be using home care services
one year after the interview. While the associations were not significant
for either the Loneliness Index or Life Space score with subsequent
use of hospitals, physician services and prescribed medications, it
might be suggested that declines in health related to social isolation
and loneliness precipitate the use of home care prior to, or instead
of, other formal care services. Results of Objective 3: Discussion and Recommendations Our final objective, to develop recommendations for policies and programs to address situations of social isolation and loneliness, was met through a method of participatory research. In conjunction with our partner organizations, we held a series of public forums in six locations throughout Manitoba. The findings from the preliminary data analyses were presented, and participants were invited to discuss their observations and concerns based on their own experiences. In general, people at the sessions felt the study findings were descriptive of situations they were aware of in their own communities and among their families. Professional caregivers also felt the information reflected the experiences of their clients. The participants discussed isolation and loneliness among older people in their communities, discussed the relevance of these issues to older people in general and older women in particular, and made suggestions for ways to address their concerns. Forum participants felt that social isolation and loneliness were more evident among those older people who:
Participants felt that social isolation and loneliness are problems relevant to older people because of:
Women’s tendency to outlive male partners and other family members, and their traditional social roles, were cited as contributing to isolation and loneliness in older age. In particular, forum participants mentioned that older women are more likely to be:
When asked if it was more likely that poor health resulted in fewer contacts with other people or if fewer contacts placed older people at greater risk of poorer health, most forum participants felt that both situations were possible. It was suggested, for instance, that those in poor health have little enthusiasm for socializing, and health conditions can be exacerbated by weather and transportation problems. It was also felt that many doctors might be unaware of the isolating effects of health problems for older individuals. It was suggested, however, that the isolation caused by declines in health might be alleviated by a move to assisted housing, or relieved temporarily by repeat contacts with health care providers. It was also felt that those who are socially isolated may be more likely to experience declines in health status because they may be at risk for decreased activity, poor nutrition, decreased mental stimulation, and may lack awareness of their health condition. Forum participants suggested several ways to address these concerns. Their recommendations are focused at three levels: for individuals, for local community agencies and groups, and for program planners and policy makers: For Individuals
For Local Community and Groups
For Program Planners and Policy Makers
Limitations and Strengths of the Research Our data are based on the one-time only responses of a representative sample of Manitobans over the age of 72, and therefore the results might not apply to younger people or those who reside in other geographic areas. Also, while our findings add to the literature concerning the relationships among isolation, loneliness and health, we were unable to explore these relationships over time. Nevertheless, our study is unique in a number of ways.
Acknowledgements
The authors acknowledge the support of the Prairie Women’s Health Centre of Excellence (PWHCE), through the Women’s Health Contribution Program, Health Canada. Please note, the views expressed do not necessarily represent the views of PWHCE or the official policy of Health Canada. Our thanks to the Normal Regional Health Authority for providing travel and accommodation for forum presenters in The Pas and Flin Flon. The Aging in Manitoba Longitudinal Study is supported by funding from
Health Canada (National Health Research and Development Program) and
Manitoba Health, and receives administrative support from the Department
of Community Health Sciences, University of Manitoba.
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
This website is copyrighted by the
Prairie Women's Health Centre of Excellence, © 1998-2011.
Website design: Pamela Chalmers E-mail: pwhce@uwinnipeg.ca. |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||